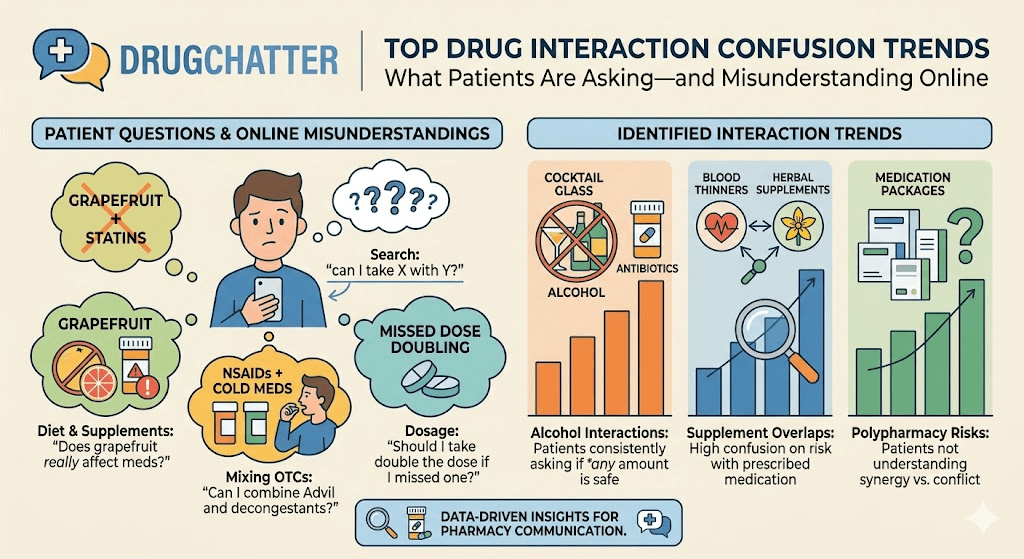
Across hundreds of patient-driven questions on DrugChatter, a clear pattern emerges: drug interactions are less about classic pharmacology errors and more about everyday life decisions—food, exercise, supplements, and overlapping medications. The result is a growing layer of confusion where clinical science meets lifestyle advice, often blurring what is actually relevant risk versus what is not.
Below are the most prominent drug interaction confusion trends shaping online discussions today, based on recent patient questions and concerns.
1. “Lifestyle interactions” are replacing traditional drug safety concerns
One of the most striking trends is the assumption that normal physical activity can change how drugs work.
Patients frequently ask whether exercise alters statin efficacy or safety—especially with widely used drugs like Lipitor (atorvastatin). Questions range from swimming and yoga to cycling and endurance training:
- https://www.drugchatter.com/chat/50680/is-lipitor-less-effective-when-swimming-regularly
- https://www.drugchatter.com/chat/21835/does-lipitor-reduce-exercise-endurance
- https://www.drugchatter.com/chat/1871/how-could-yoga-boost-lipitor-s-cardiovascular-effects
- https://www.drugchatter.com/chat/3291/lipitor-use-any-impact-on-cycling
The underlying confusion is consistent: patients often interpret muscle soreness, fatigue, or performance changes as “drug interactions,” even when no pharmacokinetic interaction exists. In most cases, these are overlapping effects of exercise physiology and statin-related muscle symptoms—not true contraindications.
Still, the frequency of these questions suggests patients are actively monitoring bodily changes and attributing them to drug behavior rather than normal variability.
2. Food and drink myths remain a dominant source of confusion
Food-drug interactions continue to generate some of the most persistent misconceptions. Grapefruit remains the symbolic villain, but nearly every category of food is now being evaluated for risk.
Examples include:
- Grapefruit alternatives and concerns: https://www.drugchatter.com/chat/63295/are-there-any-alternatives-to-grapefruit-juice-while-on-lipitor
- Dairy timing questions: https://www.drugchatter.com/chat/40369/is-it-advisable-to-consume-dairy-right-after-taking-lipitor
- Wine and alcohol interactions: https://www.drugchatter.com/chat/57661/what-are-the-effects-of-mixing-lipitor-and-red-wine
- Everyday foods like strawberries or avocados:
The recurring theme is overextension: once patients learn that some foods affect drug metabolism, they begin to suspect nearly all foods might have measurable pharmacological effects.
In reality, clinically meaningful food interactions are relatively limited and well-documented, but the online environment tends to generalize risk.
3. Supplements are now treated like “hidden drugs”
A major shift in interaction confusion comes from supplements being treated as either harmless enhancers—or secret pharmacological agents with hidden dangers.
Common questions include:
- Omega-3 and statins synergy or conflict: https://www.drugchatter.com/chat/38669/does-fish-oil-supplementation-enhance-lipitor-s-efficacy
- Probiotics affecting statin performance: https://www.drugchatter.com/chat/27895/how-do-probiotics-interact-with-lipitor-s-effectiveness
- Herbal replacements for prescription drugs: https://www.drugchatter.com/chat/20545/can-herbal-supplements-replace-lipitor-entirely
- Vitamin interactions:
The confusion here stems from a perception gap: supplements are simultaneously viewed as “natural and safe” and yet also capable of replacing or significantly altering prescription drug effects.
This dual perception leads to contradictory expectations—patients expect strong interaction effects when convenient, but minimal risk when not.
4. Statins dominate “everything interacts with everything” thinking
Lipitor appears disproportionately in interaction confusion, largely because of its ubiquity and long-term use. Many users interpret unrelated symptoms as drug interactions:
- Energy and fatigue: https://www.drugchatter.com/chat/35224/is-lipitor-effective-in-increasing-energy-levels
- Appetite and dietary behavior: https://www.drugchatter.com/chat/4854/can-lipitor-affect-your-appetite-for-morning-meals
- Protein, fat, and metabolism questions:
The underlying misconception is that statins act broadly on metabolism beyond cholesterol synthesis. In reality, atorvastatin’s mechanism is highly specific to HMG-CoA reductase inhibition, but patients often interpret systemic changes as evidence of wide metabolic disruption.
5. Combination therapy anxiety: SSRIs, NSAIDs, and blood thinners
Another major category of confusion involves drug stacking—especially when multiple commonly prescribed medications are used together.
Examples include:
- SSRIs and statins: https://www.drugchatter.com/chat/30678/lipitor-and-ssri-interaction
- NSAIDs with antidepressants and serotonin concerns: https://www.drugchatter.com/chat/61222/is-combining-advil-with-antidepressants-linked-to-serotonin-syndrome
- Blood thinners and statin bleeding risk: https://www.drugchatter.com/chat/4636/how-can-bleeding-be-prevented-while-taking-lipitor-and-blood-thinners
- General elderly polypharmacy concerns: https://www.drugchatter.com/chat/5711/how-does-lipitor-interact-with-common-elderly-medications
These questions reflect a real clinical issue—polypharmacy—but also show a tendency to overattribute risk to every combination rather than specific high-risk mechanisms.
6. “Timing logic” confusion: when drugs are taken matters—sometimes
Patients frequently assume timing can eliminate or create interactions, even when pharmacologically irrelevant.
Examples include:
- Taking Lipitor with food: https://www.drugchatter.com/chat/8828/how-does-taking-lipitor-with-food-affect-absorption
- Dairy or yogurt timing concerns: https://www.drugchatter.com/chat/28505/any-side-effects-from-eating-yogurt-with-lipitor
- Fat intake timing: https://www.drugchatter.com/chat/34046/how-does-lipitor-interact-with-fatty-food-intake
While timing matters for certain drugs (antibiotics, thyroid medications, etc.), statins generally have flexible administration rules. However, patients often apply timing logic universally, leading to unnecessary complexity in medication routines.
7. Price, access, and interaction confusion are increasingly intertwined
A newer trend shows that financial concerns are now shaping perceived drug interaction risks.
Questions about coupons, savings programs, and generics frequently overlap with safety concerns:
- Insurance coupon coverage: https://www.drugchatter.com/chat/56425/does-vascepa-coupon-cover-all-insurance-plans
- Generic Lipitor savings: https://www.drugchatter.com/chat/61195/how-much-do-i-save-with-generic-lipitor-using-insurance
- Discount cards and access programs: https://www.drugchatter.com/chat/49464/are-lipitor-discount-cards-available-at-pharmacies
The implication is subtle but important: when affordability is uncertain, patients tend to question whether cheaper versions are also “less safe” or more interaction-prone, even when bioequivalence standards are strict.
Conclusion: Interaction confusion is becoming lifestyle-centered, not pharmacology-centered
Across the dataset, the core pattern is clear: drug interaction confusion is shifting away from classic “drug A + drug B” concerns and toward a broader question—how does everything in my daily life affect this medication?
Exercise, food, supplements, finances, and routine habits are all being interpreted through a pharmacological lens. While this reflects increased patient engagement and awareness, it also introduces noise that can obscure the genuinely important interaction risks.
The challenge ahead is not just educating patients about drug interactions—but helping them distinguish between biological mechanisms and everyday coincidence.