What pharma’s regulatory, medical affairs, and brand teams need to do right now

There is a scenario playing out across millions of patient conversations every day, and almost no pharmaceutical company has a formal plan for it.
A 52-year-old woman with treatment-resistant depression opens ChatGPT on her phone. She types: ‘What medications work for depression when SSRIs have failed?’ ChatGPT responds with a detailed, confident, well-formatted answer. It names several drugs. One of them — your drug — is described as having ‘shown promise’ for her exact situation. The problem: your drug is approved for Type 2 diabetes. The ChatGPT response pulled that ‘promise’ from a 2021 preprint, a Reddit thread, and a conference abstract. She takes the information to her next doctor’s appointment, asks for it by name, and her physician — who is stretched thin and sees the printed ChatGPT output as a patient preference signal — writes the script.
That scenario is not hypothetical. It is the logical result of two simultaneous trends: the explosion of AI chatbot use for health queries, and the near-total absence of pharmaceutical industry monitoring of what those chatbots actually say about specific drugs.
By late 2024, ChatGPT reached 1.8 billion monthly visits, making it one of the top 10 most-visited sites on the planet, while Perplexity AI grew to over 100 million monthly visits by Q4 2024. Google shows AI Overviews for an estimated 84% of informational queries, and health queries rank among the most heavily affected categories. Meanwhile, a study published in JAMA Internal Medicine found that ChatGPT provided inaccurate or incomplete information in approximately 47% of drug-interaction queries.
The math is uncomfortable. Millions of health queries per day. Nearly half with material inaccuracies. Your drug almost certainly mentioned — correctly, incorrectly, or in contexts you never approved.
This article explains exactly what happens when a large language model recommends off-label uses of your drug, what the regulatory exposure looks like, and what your medical affairs, legal, and commercial teams should build right now.
How ChatGPT Actually Decides What to Say About Your Drug
Before examining the regulatory fallout, you need to understand the mechanism. ChatGPT and similar models do not retrieve information from a live database. They generate text by predicting which words are most likely to follow a given prompt, based on patterns learned from billions of documents during training.
That training corpus includes PubMed abstracts, FDA press releases, clinical trial registries, medical education websites, patient forums, Wikipedia, and yes — Reddit, Quora, and health blogs with no editorial oversight. The model has no way to distinguish ‘FDA-approved indication’ from ‘discussed in a 2019 case report.’ It synthesizes all of it into a fluent, confident-sounding response.
The pharmaceutical brands that appear most frequently and authoritatively in the training data are the ones AI mentions. Pfizer, Novo Nordisk, and AbbVie appear in thousands of peer-reviewed papers, news articles, FDA databases, and patient advocacy materials. A mid-size specialty biotech with a single approved drug in a rare disease? The model may have seen three dozen documents about that compound — mostly from a trial that failed, a patent application, and a speculative piece on drug repurposing.
This creates a fundamental asymmetry. Your brand team controls what your website says. You control your promotional materials, your sales force messaging, and your patient support content. You do not control what a 2022 preprint says. You do not control what a disease advocacy forum posted about off-label use. You do not control the training data of a model used by hundreds of millions of people.
The Training Data Lag Problem
AI training data has a lag of months to years. A drug approved by the FDA in 2025 may not appear accurately in ChatGPT’s responses until 2026 or later — if it appears at all. During that gap, patients asking AI about your new treatment get either silence or hallucinated information based on pre-approval speculation.
This lag compounds the off-label risk. When a drug is approved, there is typically years of pre-approval literature in existence — Phase II data, investigator-initiated trials in different indications, case reports in disease areas outside the label. The training corpus picks all of that up. The FDA approval notice, by contrast, is a single document. The model has no way to weight that approval as the definitive statement of appropriate use.
The result: a drug approved for Indication A may be described by ChatGPT primarily through the lens of its earlier Phase II work in Indication B — the indication that looked promising but failed to get approved. ChatGPT does not know it failed. It just sees the volume of literature.
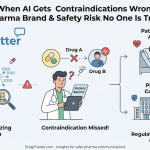
What Hallucination Actually Looks Like in Pharma Context
The word ‘hallucination’ conjures images of a model inventing drugs that do not exist. That does happen. But for established compounds, the more common and more dangerous problem is confident misattribution — the model accurately identifies a real drug, accurately describes a real condition, and then incorrectly links the two based on incomplete data.
The Vectara Hallucination Index measured factual accuracy across major LLMs and found hallucination rates ranging from 3% to 27% depending on the model and domain. Medical and pharmaceutical content consistently had higher error rates than other domains due to the complexity and specificity of drug information.
Consider a CGRP inhibitor approved for migraine prevention. Multiple research groups have investigated whether the same mechanism might address cluster headaches, a distinct and devastating condition. Preprints exist. Forum posts exist. A determined patient with cluster headaches who searches ChatGPT will likely receive information that conflates those preliminary investigations with established efficacy. The drug is real. The condition is real. The suggested therapeutic relationship is not supported by the label.
ChatGPT and other models both miss real drug-drug interactions and invent fictitious ones. In JAMA Internal Medicine testing, the system failed to flag known dangerous interactions in some cases while simultaneously warning about interactions that had no clinical basis.
The Off-Label Promotion Problem You Did Not Create
Off-label drug use is legal in the United States. Physicians can and do prescribe drugs outside their labeled indications — a practice that represents an estimated 20% of all prescriptions in the US, and substantially higher rates in oncology and psychiatry.
What is not legal is pharmaceutical companies promoting drugs for off-label uses. The Food, Drug, and Cosmetic Act prohibits manufacturers from marketing drugs for unapproved indications, and the FDA’s Office of Prescription Drug Promotion (OPDP) enforces this aggressively.
In 2025, the FDA issued more than 50 untitled letters targeting pharma DTC advertising, primarily focused on misleading imagery, minimization of risk information, and overstatements of efficacy.
The penalties for off-label promotion are substantial. GlaxoSmithKline paid $3 billion to settle charges for illegal marketing of Avandia, Paxil, Wellbutrin, and others. Pfizer paid $2.3 billion for Bextra. Eli Lilly paid $1.4 billion for Zyprexa. These are not edge cases — they are the cost of crossing lines that the FDA monitors carefully.
Now those same lines have become significantly harder to police, because the promotion is no longer coming from the company.
The Regulatory Gray Zone
When ChatGPT tells a patient that your drug is ‘highly effective for weight loss’ — even though it is only approved for type 2 diabetes — that is effectively off-label promotion happening at scale. But it is not your promotion. You did not write it, approve it, or distribute it. The AI generated it from patterns in training data.
This creates a compliance exposure that sits outside every existing regulatory framework your team has built.
The FDA’s current adverse event reporting framework — MedWatch — does not account for AI-intermediated drug information. AI responses almost never include the required risk/benefit balance that FDA mandates for promotional content.
The legal exposure has multiple dimensions:
Adverse event underreporting. If a patient harms themselves following an AI recommendation, and the AI recommendation was about your drug, the reporting chain becomes unclear. Your pharmacovigilance team is trained to pick up signals from physician reports, patient calls to your medical affairs line, and social media monitoring. An AI-generated recommendation that leads to an adverse event may never enter that chain — yet if a regulator asks whether you were aware of off-label use patterns in your patient population, your answer will be scrutinized against every signal source available.
Fair balance violations. FDA promotional rules require that any discussion of a drug’s benefits be balanced with material risk information. ChatGPT’s responses do not include fair balance. They frequently omit contraindications, black box warnings, and drug interaction data. If an AI-driven process leads to a harmful drug interaction or failed treatment, determining liability is complex. It raises critical questions about who bears responsibility — the pharmaceutical company, the software developer, or the healthcare provider.
Cross-jurisdictional inconsistency. A drug approved in the US but not in the EU will still be discussed by ChatGPT in response to European patients’ questions. The model serves a global audience but does not localize its responses to the regulatory environment of the user’s country. A recommendation that is technically defensible in the US may constitute unauthorized promotion in Germany, France, or Japan.
States like California and Colorado are rolling out laws that target AI that impersonates doctors, as well as ‘algorithmic discrimination’ in AI tools that could impact a patient’s treatment decisions. California’s AB 489, effective January 2025, requires that AI tools operating in healthcare contexts disclose their AI identity clearly and cannot use phrasing that implies a licensed healthcare provider is speaking. An AI chatbot describing your drug without that disclosure may be violating state law — and your brand may be the entity named in the subsequent news coverage, even if you had no involvement.
What the FDA Has (and Has Not) Done
In January 2025, the FDA issued a draft guidance titled ‘Considerations for the Use of Artificial Intelligence to Support Regulatory Decision-Making for Drug and Biological Products,’ providing recommendations on the use of AI to produce information or data intended to support regulatory decision-making regarding safety, effectiveness, or quality for drugs.
This guidance is important and genuinely forward-looking. It establishes a seven-step risk-based credibility assessment framework for evaluating AI models used in regulatory submissions. The FDA is thinking carefully about AI it can see — AI that pharmaceutical companies deploy in their own R&D and regulatory processes.
But there is currently no FDA guidance specifically addressing what happens when third-party general-purpose AI tools — ChatGPT, Gemini, Perplexity — describe your drug to patients without your knowledge or involvement.
As of early 2026, there is no specific FDA guidance on pharmaceutical brand representation in consumer-facing AI chatbots. This means pharma companies are operating without clear rules for a channel that is rapidly becoming a primary patient information source.
The transition to the Trump administration in January 2025 brought Executive Order 14148, which mandates a review of all AI-related policies. Under this order, agencies must reevaluate regulatory actions that might ‘impede US AI leadership.’ This policy emphasis could weaken or delay FDA’s 2025 guidance.
The international picture is equally fragmented. The EMA published a Reflection Paper in October 2024 on the use of AI in the medicinal product lifecycle, highlighting the importance of a risk-based approach for the development, deployment, and performance monitoring of AI/ML tools. But like the FDA guidance, the EMA’s work focuses on AI used within drug development — not on third-party AI tools describing approved products to patients.
The practical conclusion: you cannot wait for the FDA to solve this. The regulatory framework will eventually catch up to the behavior, but the reputational and compliance damage from off-label AI mentions accumulates now.
How AI Changes the Brand Risk Calculus
For pharmaceutical brand teams, the competitive dimension of this problem is as significant as the compliance dimension.
For a pharmaceutical brand, AI giving wrong drug information is not just a marketing problem — it is a liability exposure that your legal, medical affairs, and brand teams need to understand.
Consider what happens when your brand’s closest competitor has actively optimized its digital footprint for AI discoverability, while your brand has not. The competitor’s clinical trial results appear in well-structured, citable formats across authoritative medical publishing platforms. Your results are buried in a PDF on your corporate site, behind a cookie consent wall that AI crawlers cannot index. When a patient asks ChatGPT to compare the two drugs, the competitor appears as the obvious choice — not because its drug is better, but because its data is more accessible to the model.
Brand share in the AI layer is becoming a real and measurable variable. This is a new concept for pharma marketing teams trained entirely on the search-and-click funnel.
The Search Funnel Is Breaking
Gartner forecast in February 2024 that traditional search engine volume will drop 25% by 2026 due to AI chatbots and virtual agents. The pharmaceutical industry built its patient-facing strategy around two channels: direct-to-consumer advertising and Google search. For decades, that worked. That funnel is now breaking.
The implications cascade. A patient who would previously have typed ‘best drug for atrial fibrillation’ into Google and arrived at WebMD, then at your drug’s branded site, now asks ChatGPT directly. ChatGPT’s answer does not include a link to your site. It does not include your branded messaging. It may not mention your drug at all. Or it may mention it in the context of an indication you spent twelve years and $2 billion not pursuing.
Over 27% of US consumers had used generative AI tools like ChatGPT for health-related questions by mid-2024, according to the Rock Health Digital Health Consumer Survey. Over 70,000 health-related queries are entered into Google every minute, totaling more than 1 billion health searches per day.
The portion of those queries that now route to AI instead of traditional search is growing quarterly. Your brand’s visibility in that channel is not a future concern. It is a current business problem.
The Pharmacovigilance Signal You Are Missing
The pharmacovigilance dimension of AI-generated off-label promotion receives almost no attention in current industry discussions, and it may be the most operationally significant.
Your pharmacovigilance team monitors adverse events through a defined set of channels: spontaneous reports submitted through MedWatch, reports from healthcare providers calling your medical information line, literature surveillance, and increasingly, social media listening. That stack was designed before hundreds of millions of people started using AI chatbots as their first point of medical consultation.
Here is the gap: a patient who experiences an adverse event after following AI-generated guidance has no obvious path to report it to your pharmacovigilance team. They did not receive the drug through a physician who would file a report. They may not even know they should report anything. They asked a chatbot, got an answer, tried the drug (obtained through whatever means), and experienced a reaction. The signal simply does not enter the surveillance network.
AI’s ability to efficiently process and derive meaningful insights from both structured and unstructured data has enabled a paradigm shift from passive to active surveillance methods, allowing for real-time detection of adverse drug reactions. Despite its promise, AI implementation in pharmacovigilance faces significant challenges around ensuring data quality and representativeness, addressing potential biases in AI algorithms, and maintaining transparency.
This creates a pharmacovigilance blind spot that is structural, not accidental. The industry built its adverse event detection systems around physician-mediated drug use. AI-mediated drug use breaks that assumption entirely.
The implications extend to regulatory reporting timelines. Your regulatory affairs team is legally required to submit 15-day reports for serious, unexpected adverse events. If your surveillance systems do not capture signals from AI-influenced drug use, you may be unknowingly non-compliant — not because you concealed information, but because your monitoring architecture predates the channel.
“Medical and pharmaceutical content consistently had higher error rates in AI hallucination studies than other domains due to the complexity and specificity of drug information. Hallucination rates ranged from 3% to 27% depending on the model.” — Vectara Hallucination Index, 2024
What Your Medical Affairs Team Needs to Build
Medical affairs is the function best positioned to own this problem, and the function least likely to have a budget line for it.
The traditional medical affairs charter covers label-based scientific communication, key opinion leader engagement, medical information services, and publication strategy. None of those functions was designed to monitor third-party AI systems and correct their outputs. Building that capability requires a new mandate, new tools, and new cross-functional protocols.
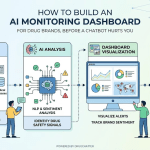
AI Mention Surveillance
The first requirement is systematic monitoring of what major AI systems say about your drug. This is not the same as social listening, though your social listening vendor may claim it is. Social listening monitors what humans say in public channels. AI mention surveillance tests what models generate in response to defined prompts — and retests regularly, because model outputs change as training data updates.
Effective AI mention surveillance requires maintaining a library of standardized test prompts that cover your drug’s approved indication, the adjacent indications where off-label use is plausible, common patient questions, and comparison queries against competitors. Those prompts should be run across ChatGPT, Gemini, Claude, Perplexity, and any AI systems embedded in patient-facing platforms in your therapeutic area.
The output is a structured log: what the AI said, what it got wrong, what indication it implied, what safety information it omitted, and whether the overall framing is consistent with your approved label.
Tools like DrugChatter are specifically built for this function — enabling pharmaceutical teams to systematically query and track AI-generated mentions of their brands across multiple models, with output structured for regulatory review. The ability to document, at a specific date and time, what a given AI system said about your drug becomes part of your pharmacovigilance and regulatory affairs record.
Cross-Functional Response Protocols
Surveillance without response is observation without action. Your medical affairs, legal, regulatory, and brand teams need a joint protocol for what happens when monitoring identifies a material discrepancy between AI-generated content and your approved label.
The protocol should answer four questions. First, does the discrepancy constitute a patient safety risk — for example, is the AI suggesting your drug for a population specifically excluded from the label due to serious adverse events? Second, is the discrepancy commercially material — is the AI consistently attributing your drug’s benefits to a competitor, or mischaracterizing your drug’s efficacy profile? Third, what corrective actions are available and appropriate — can you improve the discoverability of accurate information, or do you need to engage directly with AI platform providers? Fourth, does the discrepancy trigger any regulatory reporting obligations — for example, if you detect evidence that patients are using your drug in a way the AI recommended, and adverse events are plausible, does that constitute a signal requiring investigation?
The cross-functional nature of this protocol is essential. Pharma marketers will need to grapple with questions around bias if AI is used to personalize treatment suggestions, and smart strategies will involve creating AI guardrails that take every law into account, according to industry AI expert Nishtha Jain. Medical affairs cannot own this alone. Legal needs to be at the table when you are deciding whether an AI output constitutes off-label promotion you have an obligation to correct. Regulatory needs to be at the table when you are evaluating pharmacovigilance implications. Brand needs to be at the table when you are considering how to improve your drug’s AI visibility legitimately.
Corrective Content Strategy
Your ability to correct AI outputs about your drug is indirect. You cannot call OpenAI and ask them to update ChatGPT’s answer. What you can do is improve the quality, authority, and discoverability of accurate information in ways that are more likely to influence future model training and retrieval.
Some pharma brands are using AI content tags and digital watermarks, while others are partnering with platforms where patients and providers can access verified, evidence-based information from licensed professionals. These are nascent strategies, but they reflect a correct directional instinct: the goal is to make accurate information about your drug more prominent and more parseable in the sources AI models use.
Practically, this means structuring your clinical publications for machine readability — using structured abstracts, clear indication statements, and explicit safety language that a model can extract cleanly. It means ensuring your prescribing information is hosted on authoritative, crawlable domains in formats that AI systems can access. It means generating content on platforms that have high credibility in medical AI training data — major medical journals, FDA databases, established patient advocacy organizations.
In today’s climate, safety signals, misinformation, and regulatory sentiment often emerge through public discourse first. Modern social intelligence and pharmacovigilance approaches need to be proactive and context-aware, providing brands with reassurance and strategic insights.
The Legal Landscape in 2025 and 2026
The legal exposure from AI-generated off-label drug mentions sits at the intersection of product liability, promotional compliance, and a new and largely untested regulatory category.
Traditional product liability doctrine assigns responsibility to manufacturers when their products cause harm. Courts have applied this doctrine through negligence, strict liability, and failure-to-warn theories. Applying these doctrines to black-box AI systems — where the rationale behind an algorithm’s decision-making may be opaque or incomprehensible even to its creators — poses significant challenges. One potential path forward involves mandating transparency and auditability as preconditions for regulatory approval.
The failure-to-warn theory is most relevant to pharmaceutical companies. Historically, drug manufacturers must ensure that adequate warnings accompany their products’ use. Off-label use that a manufacturer knew or should have known about can create a duty to warn — even for uses the company never promoted. If AI systems are now a significant driver of off-label use at scale, the argument that manufacturers ‘should have known’ becomes increasingly plausible once the monitoring tools exist to detect it.
This is not hypothetical. The Off-Label Promotion settlements discussed earlier — GlaxoSmithKline’s $3 billion, Pfizer’s $2.3 billion, Eli Lilly’s $1.4 billion — were based in part on the government’s ability to demonstrate that manufacturers had knowledge of off-label use patterns and continued to benefit commercially from them. AI monitoring creates a documented record of what off-label narratives existed in the AI ecosystem and when. A company that monitors and does nothing may face greater exposure than a company that never monitored — because the record will show they knew.
State-Level AI Regulation Creates New Compliance Obligations
While no federal law overseeing AI in healthcare currently exists, regulators can rely on a deep well of existing laws — from data privacy laws like HIPAA to the Food, Drugs and Cosmetic Act — to address concerns about how pharma marketers are using AI.
California’s AB 489, effective January 2025, is the clearest current example. It prohibits AI tools operating in healthcare contexts from implying they are licensed healthcare providers and requires clear disclosure. But the law’s scope includes not just tools deployed by healthcare providers, but tools that operate in a healthcare context — which could encompass any AI system regularly used to answer drug questions.
Colorado’s equivalent legislation follows a similar principles-based approach focused on preventing algorithmic discrimination in treatment decisions. As more states pass AI-specific laws in 2025 and 2026, pharmaceutical companies will face a patchwork of state obligations that interact unpredictably with federal regulatory requirements.
The practical response is to build compliance monitoring that operates across jurisdictions — tracking not just what AI says about your drug, but what regulatory context applies to each instance of that statement.
GLP-1s, Oncology Drugs, and High-Volume Off-Label Targets
Some therapeutic categories face this problem acutely.
GLP-1 receptor agonists — semaglutide (Ozempic, Wegovy), tirzepatide (Mounjaro, Zepbound) — have generated more AI conversation than almost any other drug class. The off-label weight loss use of Ozempic became a cultural phenomenon before Wegovy received approval for obesity. ChatGPT’s training corpus is saturated with content from that period. The model routinely discusses weight loss in the context of drugs approved only for type 2 diabetes, because that is what the training data reflects.
Novo Nordisk’s situation is instructive. The company’s approved obesity indication for semaglutide is Wegovy, not Ozempic. But ChatGPT frequently conflates the two or describes Ozempic as a weight-loss drug without appropriate qualification. This is not a fabrication — it reflects the reality of how the drug was used and discussed before formal approval. But from a regulatory standpoint, it creates promotional content that Novo Nordisk cannot control and would never approve.
The oncology space presents a different version of the same problem. Targeted therapies approved for specific biomarker-defined populations get discussed in AI responses for the broader cancer type, regardless of biomarker status. Pembrolizumab (Keytruda) is approved for tumor-agnostic use in patients with specific biomarker profiles — but AI responses frequently describe it in ways that imply broader utility than the label supports. For oncology brands, this creates the dual risk of off-label patient expectations and inappropriate prescribing signals to physicians who use AI tools in their practice.
Psychiatry is the third high-risk area. Drugs approved for one psychiatric indication get discussed extensively in the context of others — ketamine derivatives approved for treatment-resistant depression discussed as potential treatments for PTSD, antipsychotics approved for schizophrenia discussed in the context of bipolar depression management, and so on. The psychiatric evidence base generates enormous volumes of academic and patient forum discussion, all of which trains AI models without any mechanism for label compliance.
What AI Platform Providers Are (and Are Not) Doing
Understanding the counter-party in this situation is important. OpenAI, Google, Anthropic, and Perplexity are aware that their systems generate health information at scale. They have taken steps to address the most obvious risks — adding safety disclaimers to responses about self-harm, refusing to provide detailed instructions for dangerous activities, and indicating when the user should consult a doctor.
What they have not done is build pharmaceutical label compliance into their medical response architecture. They cannot. They do not have access to a continuously updated database of every drug’s approved indications and corresponding safety information, linked to the jurisdiction of the user. Building that infrastructure would require either a regulatory-grade data partnership with entities like the FDA, DailyMed, or a commercial drug information provider — or a custom verification layer for every medical claim.
Some models do attempt retrieval-augmented generation — supplementing their base knowledge with real-time searches of authoritative sources. When this works, it can produce more current and accurate drug information. When it does not work, it can produce a response that cites an authoritative source while getting the substance of that source wrong.
The bottom line for pharmaceutical companies: do not assume that AI platform providers will solve this problem. They may improve their medical information accuracy over time, but their incentive is to provide helpful responses to users, not to enforce pharmaceutical promotional compliance. Those goals are not the same thing.
Building an AI Visibility Strategy: The Practical Steps
Pharmaceutical companies need a structured approach to AI brand monitoring, and they need it to operate within existing regulatory frameworks while building new capabilities. Here is a four-part framework.
Step 1: Establish Your AI Footprint Baseline
Before you can monitor drift, you need to know where you are. Commission a baseline audit of how your drug appears across major AI systems. Use standardized prompts — one set covering your approved indication, one covering adjacent indications where off-label use is plausible, one covering patient-type questions (‘Is [drug name] right for me?’), and one covering physician-type questions (‘What is the recommended dosing of [drug name] for [condition]?’).
Document the results with timestamps and model version information. This baseline becomes your reference point for change detection and your evidence base if a regulatory question ever arises about your awareness of AI-generated information.
Step 2: Assign Cross-Functional Ownership
AI mention surveillance is not a marketing project. It is not a social listening project. It is a compliance and pharmacovigilance function that happens to have brand implications. In most pharmaceutical organizations, the function that has the regulatory authority and the obligation to act on drug safety information is medical affairs — specifically, the medical information and pharmacovigilance functions.
Medical affairs should lead the ownership structure, with defined escalation paths to regulatory affairs, legal, and commercial for different types of findings. The pharmacovigilance team needs to have input on signal assessment protocols. Legal needs to review the monitoring methodology to ensure it does not inadvertently create obligations the company cannot meet.
Step 3: Build Corrective Content Infrastructure
Your drug’s accurate information needs to be accessible to AI systems in formats they can use. This means:
Structured prescribing information on authoritative, publicly accessible domains with clean HTML markup. AI crawlers do not parse PDFs well. If your prescribing information exists only as a PDF on your corporate site behind a pop-up modal, it is effectively invisible to model training pipelines.
Structured clinical data abstracts published on platforms with high authority in AI training data — PubMed, ClinicalTrials.gov, FDA press releases. Every abstract should include explicit indication language, patient population definitions, and safety information.
Patient-facing content that is factually precise and AI-parseable. Marketing language designed to evoke emotional response is poorly suited to AI extraction. Clear, direct statements of what the drug does, for whom, and under what conditions — the kind of language that sounds overly clinical for traditional advertising — is what AI models can accurately extract and reproduce.
Step 4: Monitor, Compare, and Escalate
Establish a regular monitoring cadence — monthly at minimum, weekly for newly launched drugs or drugs in therapeutic areas with high AI conversation volume. Compare current outputs against your baseline. Flag deviations for cross-functional review. Build a formal escalation path for safety-relevant findings.
Tools like DrugChatter are designed specifically to support this workflow — providing structured query capabilities across multiple AI platforms, with outputs formatted to support medical affairs documentation and pharmacovigilance reporting. The ability to demonstrate, at a specific date and time, what a given AI system said about your drug, and to compare that against your approved label, is becoming a standard expectation for pharmaceutical regulatory affairs teams operating in the AI age.
The Competitive Intelligence Dimension
AI monitoring is not only about defense. The same systems that might describe your drug inaccurately may describe your competitors’ drugs accurately — or vice versa. Understanding how AI positions your drug relative to competitors across multiple query types gives you commercially valuable information that is not available through any other channel.
Traditional brand tracking surveys measure physician recall and patient preference at the moments when you conduct the survey. AI monitoring gives you a continuous signal of how the informational ecosystem positions your drug. If AI consistently recommends your competitor first for a query type that represents 40% of your commercial opportunity, that is a commercially material finding that warrants a strategic response — improving your content infrastructure, generating more authoritative publications, building relationships with the medical information platforms that feed AI training data.
The possibility of AI misinterpreting or misquoting brand claims poses legal risk. To mitigate this, some pharma marketers are revisiting their MLR review processes, incorporating LLM simulators during content development to test how AI models interpret their messaging.
This practice — running your content through an LLM during the MLR review process to see how the model will parse it — is a legitimate and increasingly necessary quality check. If your approved promotional content generates an inaccurate AI summary when fed into a model, that is information your MLR committee needs before the content goes live.
What Happens When Patients Bring AI Recommendations to Physicians
The scenario at the start of this article — a patient printing a ChatGPT response and bringing it to a physician visit — is already happening at scale. A 2024 survey by the American Medical Association found that a growing minority of patients arrive at appointments having consulted AI tools, and that physicians report increasing pressure to address AI-generated health information.
For pharmaceutical companies, this creates a physician education obligation. Your medical science liaisons need to be equipped to address AI-generated off-label claims in their discussions with healthcare providers. This requires knowing what the AI is actually saying — which brings the monitoring function back to the center.
The physician side of this interaction is its own regulatory consideration. A physician who prescribes based on AI-generated information, where that information was factually inaccurate, may have a defense based on reliance on an apparently authoritative source. The question of whether your company had an obligation to correct that source — and failed to — is one that plaintiff attorneys in future pharmaceutical liability cases will raise.
When signals are distorted at the detection stage, the downstream impact on causality assessment can be profound. Causality assessment in pharmacovigilance relies not only on the signal itself but on a comprehensive understanding of case-level detail, confounding variables, and background incidence rates. AI systems with incomplete data can obscure key temporal associations and reduce the ability to apply structured algorithms with confidence.
The Opportunity Inside the Risk
Pharmaceutical companies that get ahead of this problem gain a genuine competitive advantage. The majority of the industry is still treating AI as a content generation tool for internal use — a way to draft clinical documents faster, summarize literature, or support market access submissions. The minority that also treats AI as a brand and compliance monitoring channel will have capabilities that the majority lacks when the regulatory scrutiny arrives.
The first companies to build systematic AI mention monitoring will have the strongest documentation of their awareness and response to off-label AI content. They will have the clearest understanding of their AI brand positioning. They will have the most developed protocols for cross-functional response. And when the FDA eventually provides formal guidance on AI-generated drug information — which it will — they will have the internal infrastructure to comply quickly while their competitors scramble to build from scratch.
The market for AI in pharmaceuticals is projected to grow from $1.94 billion in 2025 to approximately $16.49 billion by 2034. Companies that harness AI effectively are achieving faster R&D pipelines, better engagement with healthcare providers, and more agile operations.
The same infrastructure that makes AI a competitive advantage in R&D can make it a competitive advantage in brand protection — if pharmaceutical companies choose to build it.
Key Takeaways
The scale of AI health queries is large and growing. Over 27% of US consumers used AI for health questions by mid-2024. ChatGPT reached 1.8 billion monthly visits by late 2024. Your drug is being discussed in AI responses without your knowledge or consent.
AI off-label mentions constitute a regulatory gray zone with real exposure. There is no FDA guidance specifically addressing third-party AI chatbot representations of pharmaceutical brands. The existing framework for off-label promotion, adverse event reporting, and fair balance does not map cleanly to AI-generated content. That gap is a compliance risk, not a safe harbor.
Pharmacovigilance systems have a structural blind spot. Adverse event surveillance was designed for physician-mediated drug use. AI-mediated drug use creates a parallel pathway where patients act on AI recommendations without entering the established reporting chain.
Your corrective options are indirect but real. You cannot directly edit AI outputs. You can systematically improve the quality, authority, and machine-readability of accurate information about your drug, which influences future model training and retrieval. This requires treating content quality as a pharmacovigilance and compliance function, not just a marketing function.
Cross-functional ownership is essential. Medical affairs, regulatory, legal, and commercial teams all have a stake in AI mention monitoring. Medical affairs should lead, with defined escalation protocols for different finding types.
Monitoring creates a documentation record with regulatory implications. Companies that monitor and document what AI systems say about their drugs will have evidence of their awareness and response. That documentation may become important in regulatory and legal proceedings. Companies that do not monitor will not have a defense based on ignorance — they will simply have no record at all.
Competitive intelligence is a secondary benefit. AI monitoring reveals how your brand is positioned relative to competitors across multiple query types — a continuous signal that traditional brand tracking cannot provide.
The regulatory environment is moving. FDA, EMA, and state regulators are all actively developing frameworks for AI in healthcare. Companies that build internal governance now will be positioned to comply quickly when formal guidance arrives.
FAQ
Q: If a patient experiences an adverse event after following an AI chatbot’s off-label drug recommendation, does my company have any legal exposure?
A: Potentially yes, though the legal theory is still developing. The failure-to-warn doctrine has historically been applied to situations where a manufacturer knew or should have known about off-label use patterns. If your company has access to monitoring tools that would reveal AI-generated off-label content — and either chose not to monitor or monitored and did not act — a plaintiff’s attorney will argue constructive knowledge. The liability question is complicated by the fact that OpenAI, not your company, generated the recommendation. But courts assessing pharmaceutical liability look at the whole chain of events, and your failure to correct a known inaccuracy about your product may be relevant to that assessment. This is an area where pharmaceutical legal teams need proactive guidance now, before the first case law develops.
Q: Can I contact AI companies like OpenAI directly to correct inaccurate information about my drug?
A: You can contact them, and some AI companies have established channels for factual corrections from authoritative sources. But the path from ‘we submitted a correction’ to ‘ChatGPT now responds accurately’ is indirect, slow, and not guaranteed. Model retraining cycles are infrequent. Retrieval-augmented systems may update more quickly if you improve the quality of source documents they retrieve from. The most reliable strategy is to systematically improve the quality and discoverability of accurate information in the source documents AI systems use — FDA databases, PubMed, authoritative patient education platforms — rather than relying on direct corrections to model providers.
Q: My drug is in a rare disease indication with very little online discussion. Does AI mention risk still apply to me?
A: It applies differently. For rare disease drugs with limited online footprint, the risk of AI discussing your drug at all may be low — which means patients are not getting inaccurate AI information, but they are also not getting accurate information when they need it. The more immediate risk is that AI describes a competing treatment, or a legacy treatment in your disease area, while failing to mention your approved therapy. That is an AI visibility problem as much as a compliance problem. Rare disease companies should audit not just what AI says about their drug, but whether AI mentions their drug at all when asked about treatment options for their disease.
Q: How should I position AI mention monitoring within my organization? Which team owns it?
A: Medical affairs is the natural owner because the function carries legal responsibility for scientific communication about the drug. Specifically, the medical information and pharmacovigilance functions within medical affairs have the clearest regulatory mandate to be aware of how their drug is discussed and to respond to safety-relevant inaccuracies. The monitoring function should be formally chartered, with a defined scope, a regular cadence, a cross-functional review committee, and an escalation protocol. Building it as an informal project within digital marketing underestimates the regulatory obligation and almost guarantees it will be deprioritized when budget cycles tighten.
Q: What does ‘voice of the customer’ mean in the context of AI monitoring, and how can it help my brand strategy?
A: Traditional voice of customer research captures what patients and physicians say when you ask them specific questions through surveys, interviews, or advisory boards. AI monitoring captures what questions patients are actually typing — unmediated, spontaneous, and at scale. If you monitor the questions people ask AI chatbots about your therapeutic area, you get a direct signal of patient concerns, misconceptions, and decision criteria that your brand team may not have known existed. A patient who asks ‘Can [your drug] cause hair loss?’ is revealing an unmet information need. A patient who asks ‘Is [your drug] better than [competitor] for people who travel frequently?’ is revealing a quality-of-life concern that your clinical messaging may not address. This information is commercially valuable independent of the compliance dimension, and it represents one of the more immediate ROI arguments for building AI monitoring capability.
DrugChatter is a pharmaceutical intelligence platform built to help drug companies systematically monitor, document, and respond to AI-generated mentions of their brands across major language models. The platform is designed specifically for medical affairs, regulatory, and pharmacovigilance teams operating within pharmaceutical compliance frameworks.