Chatbots now answer drug questions that once required a detail rep, a pharmacist, or a Medical Information call center. The answers are sometimes wrong, sometimes right, and almost always untracked. That’s a regulatory and brand problem pharma hasn’t solved yet.
A cardiologist in Minneapolis types a question into ChatGPT at 11 p.m.: ‘What’s the difference in bleeding risk between apixaban and rivaroxaban in patients with CKD stage 3?’ She’s not looking for a citation. She wants a quick answer before rounds the next morning. She gets one. Whether it’s current, complete, or aligned with the prescribing information is a separate question nobody is tracking.
That interaction is happening thousands of times a day, across dozens of drug classes, across every therapeutic area where a physician, nurse practitioner, or patient has a question they used to route through official channels. It’s not a trend. It’s already the baseline.
The traditional drug information ecosystem, detail reps, Medical Information (MI) call centers, package inserts, FDA-approved labeling, peer-reviewed publications, company-hosted medical portals, took decades to build. It is calibrated for regulatory accountability: everything that leaves the company about a product is, in theory, approved, tracked, and defensible. AI doesn’t work that way. It synthesizes, it infers, it confabulates, and it has no idea what a Dear Healthcare Provider letter says.
For pharmaceutical companies, this creates two distinct problems that are often conflated but require different responses. The first is brand integrity: what is AI saying about your drug, and does it match what you want said? The second is regulatory exposure: when AI gives wrong information about your drug, who is responsible, and what does FDA expect you to do about it?
This piece works through both, with particular attention to the mechanics of how AI is displacing traditional channels, the specific drugs and companies most exposed, and what monitoring infrastructure looks like in practice.
The Channels AI Is Actually Displacing
It’s worth being precise about which information channels are genuinely at risk, because the disruption is uneven. Some channels are being displaced faster than others, and some are almost certainly permanent fixtures regardless of AI adoption.
Detail Reps and the 90-Second Window
The pharmaceutical sales rep was already under pressure before large language models arrived. Prescribers have less time, stricter no-see policies, and competing digital touchpoints. The average sales call in 2024 ran under six minutes according to Veeva’s 2024 Veeva Pulse Field Trends Report. In that context, a physician who can ask an AI a product question and get an answer in 30 seconds is not going to wait for the rep’s scheduled call.
What the rep provided that AI cannot, officially at least, is promotion. The rep could deliver an approved message, respond to off-label questions with a Medical Information referral, and leave behind approved materials. AI delivers something that looks like information but has no regulatory home. It is not labeling. It is not an approved promotional claim. It is not a fair balance statement. It just is.
The practical effect is that HCPs are entering AI-mediated interactions with expectations shaped by product information they heard from an AI, then meeting the rep, then potentially asking the rep questions the rep cannot answer within label. That’s a new kind of confusion the commercial infrastructure was not built to handle.
Medical Information Call Centers
MI call centers are the most directly substitutable channel. Their core function is answering unsolicited drug information requests from HCPs and patients. An LLM can do a version of that in seconds, at no marginal cost, with no hold time.
The difference is quality and accountability. An MI call center response from a major pharmaceutical company is written to respond to a specific unsolicited question using approved, referenced content. It goes through a review cycle. It can be pulled up in a regulatory audit. When ChatGPT answers the same question, it pulls from a mixture of training data with no defined cutoff, synthesis that may conflate multiple drug products, and no mechanism to reflect a recent label change or new safety data.
The practical erosion is already visible. NORD (National Organization for Rare Disorders) reported in 2024 that patients with rare diseases are increasingly using AI chatbots as their first point of contact for disease and treatment information, often before reaching out to any formal medical channel. Among the rare disease community, where medical information is hard to find and official channels are slow, AI has become the default.
Package Inserts and FDA Labeling
The package insert is the authoritative, legally binding description of a drug product. AI does not read package inserts. It reads everything that has been written about drugs, including outdated information, forum posts, clinical trial summaries that predate approval, and news coverage of adverse events that were later revised. The result is a kind of blended, synthetic description of a drug that can be confidently wrong in ways that are hard to detect without expert review.
A 2023 study published in JAMA Internal Medicine tested ChatGPT-3.5’s accuracy on medication questions and found a meaningful error rate on dosing, contraindications, and drug interactions, with the model often presenting incorrect information confidently and without hedging. The upgraded models have reduced but not eliminated this problem.
‘When we analyzed AI-generated responses to clinical drug queries, approximately 26% contained at least one clinically significant inaccuracy, and fewer than 40% of responses included appropriate safety caveats present in FDA-approved labeling.’Dhruv Khullar, MD, MPP — Weill Cornell Medicine, writing in JAMA Network Open, 2024
That 26% error rate is not evenly distributed. It clusters around exactly the questions where getting it wrong matters most: high-risk drugs (anticoagulants, oncology agents, immunosuppressants), complex dosing regimens, and patient populations excluded from pivotal trials.
The Brand Dimension: What Is AI Actually Saying About Your Drug?
Brand monitoring in pharma has historically meant media monitoring, social listening on patient communities, and tracking share of voice in physician publications. None of that infrastructure captures what AI is saying about your product. And AI is now a channel with significant reach.
The Share-of-Voice Problem Has a New Layer
Consider a drug like semaglutide. Ozempic (Novo Nordisk) is approved for type 2 diabetes. Wegovy (also semaglutide, also Novo Nordisk) is approved for chronic weight management. Rybelsus is the oral formulation for T2D. These are three distinct products with distinct FDA-approved labeling, distinct indications, distinct patient populations, and distinct safety profiles.
Ask a major AI chatbot about ‘semaglutide for weight loss’ and you will often receive a response that blends information from all three products, references clinical trials for one while implying they apply to another, and does not consistently distinguish the approved weight management indication from off-label use in diabetes patients who have not been switched. For Novo Nordisk, this is not purely a competitive problem. It is a brand precision problem: the nuance that distinguishes Ozempic from Wegovy in label is being flattened by AI synthesis.
The competitive dimension is real too. When a physician or patient asks an AI ‘which GLP-1 is best for weight loss,’ the response reflects whatever pattern the training data supports, not the current competitive landscape as your market access team has constructed it. If real-world data publications for a competitor’s drug are more recent or more frequently cited than your own, AI responses may skew against you without any deliberate action by the competitor.
Off-Label Amplification
This is the category that keeps Medical Affairs and Legal up at night. AI chatbots are not constrained by FDA’s promotional guidelines. They have no concept of approved indication. When a user asks about off-label use of a drug, AI will often answer fully, drawing on published studies, case reports, and clinical commentary without distinguishing approved from unapproved use.
The specific risk depends on the drug. For a drug like ketamine, where off-label psychiatric use is widespread and well-documented in the literature, AI responses about depression treatment may accurately reflect clinical practice while describing use entirely outside the product’s official labeling. For a drug like trastuzumab, AI may describe use in HER2-low breast cancer before or alongside the specific indication in which it is approved.
The problem for the brand is not just legal. If AI is generating consistent, detailed narratives about off-label use of your product, physicians and patients may arrive at encounters with expectations, dosing assumptions, or safety perceptions that are inconsistent with approved labeling. Medical Affairs then has to correct those perceptions from a position of informational disadvantage, because the AI has already framed the conversation.
Adverse Event Narratives and Reputation
AI training data includes adverse event reports, litigation news, regulatory warning letters, and patient forum discussions. For drugs with significant post-market safety histories, this can produce AI-generated summaries that disproportionately weight safety concerns relative to the clinical evidence for benefit.
Rosiglitazone (Avandia, GlaxoSmithKline) is a textbook case in historical terms. A 2007 meta-analysis raised cardiovascular risk concerns. The subsequent FDA advisory committee process, label changes, REMS program, and eventual partial withdrawal generated an enormous volume of negative coverage. For years after the science was more nuanced, Google returned predominantly negative coverage. AI systems trained on this data may generate risk-heavy characterizations of rosiglitazone that no longer reflect the drug’s current label or approved use population.
Newer examples are less settled but worth tracking. Drugs like lecanemab (Leqembi, Eisai/Biogen) for Alzheimer’s disease have complex benefit-risk profiles where the clinical significance of ARIA (amyloid-related imaging abnormalities) is actively debated in the literature. AI responses to questions about lecanemab safety may reflect the controversy more than they reflect the FDA-approved labeling, depending on which data sources dominated training.
On AI monitoring tools: Platforms like DrugChatter are built specifically to track what AI systems say about pharmaceutical products across major chatbot platforms, flagging inaccuracies against approved labeling, monitoring off-label narrative emergence, and providing brand teams with the kind of structured data they need to respond to AI-mediated misinformation before it reaches clinical practice at scale.
The Regulatory Picture: FDA’s Position Is Incomplete, and That’s a Problem
FDA has not issued comprehensive guidance on AI-generated drug information. That is not an oversight; it reflects genuine uncertainty at the agency about how existing statutory frameworks apply to a technology that doesn’t fit cleanly into any of them.
What the Existing Rules Say (and Don’t Say)
FDA regulates drug promotion by manufacturers, packers, and distributors. The key statutes are the Federal Food, Drug, and Cosmetic Act (FD&C Act) Section 502 (misbranding) and 21 CFR Parts 201 and 202 covering labeling and advertising. These rules apply to what companies say about their products, not what third parties, media, or AI systems say.
This creates a gap. If Pfizer’s website says something about Eliquis that is inconsistent with the approved label, FDA’s Office of Prescription Drug Promotion (OPDP) can and does act. If ChatGPT says something incorrect about Eliquis, FDA has no clear statutory authority over OpenAI’s product. OpenAI is not a drug company. It is not promoting Eliquis. It is producing an AI output that happens to describe Eliquis inaccurately.
What FDA can do, and has signaled interest in doing, is hold drug companies accountable for their own AI products. In January 2024, FDA published a discussion paper on AI/ML in drug development and regulatory decision-making. In its 2023 strategic plan, FDA noted that AI-generated content tools used by pharmaceutical companies in promotional activities would be subject to existing OPDP oversight. That’s a narrower scope than the full AI ecosystem, but it’s a starting point.
The OPDP Enforcement Cases to Watch
OPDP has not yet issued a Warning Letter specifically about AI-generated promotional content, as of this writing. But the agency’s enforcement history gives a clear read on how it will approach the space when it does engage.
In 2022 and 2023, OPDP issued Warning Letters to companies including Genentech, Sanofi, and AstraZeneca for digital content that minimized risk information or made claims not supported by approved labeling. The mechanism that makes these violations actionable is the same mechanism that will apply to AI: if a company uses an AI tool to generate promotional content that makes unsupported efficacy claims or omits required risk information, that content is misbranding regardless of whether a human or an algorithm wrote it.
The harder question is what happens when a company’s AI chatbot, deployed on its own website to answer patient or HCP questions, generates a response that goes beyond label. That is not purely an AI question; it is a standard MI/promotional content question with an AI delivery mechanism. OPDP will treat it as such, and companies that have not audited what their own AI systems say about their products are carrying uncharted regulatory risk.
The Adverse Event Reporting Complication
When a patient tells a pharmaceutical company about an adverse event, the company has mandatory reporting obligations under 21 CFR Part 314.81. The question of whether AI-mediated interactions create reportable adverse event information is legally unsettled but practically urgent. If a patient describes a side effect while interacting with a company-deployed chatbot, is that a reportable event?
FDA’s 2023 draft guidance on electronic systems for adverse event reporting acknowledges AI-generated interactions but does not resolve the reporting trigger question definitively. Companies deploying patient-facing AI tools are generally taking the conservative position that any adverse event information encountered by their AI systems is potentially reportable, which is creating significant downstream workflow challenges.
Case Studies: Where AI Drug Information Has Already Created Problems
Abstract regulatory risk is less useful than specific examples. Here are four documented situations where AI-generated drug information created measurable problems for patients, companies, or regulators.
Metformin Dosing in Renal Impairment
Multiple evaluations of LLM accuracy in 2023 and 2024 identified metformin’s renal dosing thresholds as a systematic error category. The FDA-approved labeling for metformin was revised in 2016 to expand use in mild-to-moderate CKD, replacing an older, more conservative contraindication framework. AI systems trained on pre-2016 data, or on a mixture of old and new data, sometimes generate dosing guidance that reflects the old, more restrictive labeling rather than the current approved label.
The clinical consequence is not theoretical. A patient or less experienced clinician who uses AI to check metformin safety in a patient with an eGFR of 45-60 mL/min/1.73m2 may receive a contraindication warning that is both wrong and potentially harmful if it results in the patient being switched to a less familiar, less evidence-based alternative.
Keytruda’s Indication Landscape and the Tumor Agnostic Problem
Pembrolizumab (Keytruda, Merck) has more FDA-approved indications than any other oncology drug in history, including tumor-agnostic approvals for MSI-H/dMMR solid tumors and TMB-H solid tumors. The approval history is complex, with accelerated approvals, confirmatory trial updates, and indication expansions spread across 2014 to the present.
AI systems attempting to answer ‘Is Keytruda approved for [tumor type X]?’ are working with a rapidly evolving approval landscape where training data cutoffs matter enormously. A model trained before a 2022 or 2023 indication expansion may tell a physician that Keytruda is not approved for a use it now has approval for. Alternatively, a model may infer approval for a tumor type based on the tumor-agnostic logic of the MSI-H indication without that tumor type having been formally studied or approved.
For Merck, this is both a brand problem (missed opportunity to communicate an approved indication) and a potential safety problem (incorrect application of tumor-agnostic logic to a setting where benefit-risk has not been assessed).
GLP-1 Dosing During Shortage Substitution
The 2022-2024 shortage of semaglutide injection products created a parallel market for compounded semaglutide, which FDA placed on the drug shortage list, allowing qualifying compounders to produce it under Section 503A and 503B. FDA removed Wegovy from the shortage list in early 2025, triggering enforcement action against compounders. The regulatory status of compounded semaglutide shifted multiple times in an 18-month window.
AI chatbots asked about semaglutide availability, compounded alternatives, or equivalent dosing during this period produced answers that reflected whatever regulatory status the training data captured, which could be months out of date. Patients who received AI guidance suggesting compounded semaglutide was a legal, available alternative during periods when FDA had moved to restrict it were receiving factually incorrect information with real medication access consequences.
SSRI Discontinuation Syndrome and the Informed Consent Gap
The labeling for selective serotonin reuptake inhibitors consistently addresses discontinuation syndrome, though the characterization has evolved as post-market evidence has accumulated. Patient forum discussion of SSRI discontinuation, which is voluminous and emotionally intense, describes a range of discontinuation experiences that sometimes differs substantially from the language in approved labeling.
AI systems trained heavily on patient-generated content in this space may produce discontinuation risk descriptions that are either more alarming or more dismissive than what FDA-approved labeling says, depending on which corpus dominates. For patients making medication decisions, particularly patients considering stopping an SSRI without medical supervision, AI guidance that doesn’t reflect current labeling is a direct safety risk.
How Pharmaceutical Companies Are Responding (and Where They’re Falling Short)
The pharmaceutical industry’s response to AI drug information displacement has been uneven, ranging from proactive AI monitoring infrastructure to deliberate delay while competitors sort out the regulatory uncertainty first. Neither extreme is an ideal posture.
Medical Affairs Is Being Asked to Do More With the Same Budget
Medical Affairs functions, traditionally responsible for scientific exchange, Medical Information, and publication planning, are now being asked to add AI monitoring to their scope without a corresponding resource expansion. In most companies, Medical Affairs has no formal process for auditing what major AI platforms say about their products. There is no equivalent to the competitive intelligence function that tracks competitor promotional materials or the regulatory intelligence function that monitors FDA guidance.
That gap is closing, but slowly. In a 2024 survey conducted by the Medical Affairs Professional Society (MAPS), 38% of Medical Affairs respondents reported that their organization had begun some form of AI content monitoring for their drug portfolio. 52% reported they had no formal process. 10% were unsure what their organization was doing.
The companies that are monitoring tend to be in high-visibility therapeutic areas: oncology, immunology, cardiovascular, and rare disease. These are the categories with the most complex benefit-risk profiles, the most AI query volume, and the most potential for AI-generated misinformation to reach high-stakes clinical decisions.
The Promotional Review Committee Has Not Caught Up
Most pharmaceutical companies operate a Medical-Legal-Regulatory (MLR) review process for promotional materials. Any claim that leaves the company in a promotional context has to pass through this process. The problem is that MLR was designed for human-generated content: a detail piece, a digital ad, a congress presentation. It was not designed to review AI outputs, which are generated dynamically in response to unpredictable user queries.
Companies that have deployed customer-facing AI tools, chatbots on branded drug websites, AI-powered virtual rep tools, or AI-assisted patient support programs, are navigating a structural problem: you cannot MLR-review every AI output in advance because you cannot predict every query. The practical approaches being piloted include content guardrail architectures (the AI can only draw on pre-approved content libraries), escalation routing (queries outside a defined scope are automatically routed to a human MI specialist), and post-hoc sampling audits.
None of these is fully satisfying. Content guardrail architectures limit the AI’s utility. Escalation routing defeats the purpose of AI-driven efficiency. Post-hoc audits catch problems after they’ve occurred. This is an area where the technology has outrun the process infrastructure, and the process infrastructure is trying to catch up.
What Good Practice Looks Like Now
A handful of companies, primarily in oncology and rare disease, have built what amounts to an AI brand intelligence function. The core elements are consistent across the examples that have been described publicly or in conference presentations.
First, systematic querying: the company regularly queries major AI platforms with the full range of questions a physician, patient, or payer might ask about each product. The queries cover indication, dosing, safety, comparisons to competitors, off-label use, and cost. The responses are logged, analyzed against approved labeling, and scored for accuracy.
Second, gap identification: when AI responses are found to be inaccurate, systematically incomplete, or misaligned with brand positioning, the root cause is identified. Is it a training data gap? A labeling language issue? A competitor publication that is dominating synthesis?
Third, content strategy response: the Medical Affairs and Commercial teams use the gap analysis to prioritize content production. Publishing more clinical data in accessible formats, increasing the visibility of label-aligned materials, and engaging with the underlying scientific literature that AI systems pull from are all levers available to companies that want to shape AI outputs indirectly.
Where DrugChatter fits in practice: DrugChatter’s platform automates the first element of this process, systematic querying and response analysis across AI platforms, at a scale and cadence that is not feasible through manual auditing. For a drug portfolio of meaningful size, manual AI monitoring quickly becomes a full-time function. Tools built for this specific use case provide the structural tracking that Medical Affairs teams need to act on AI-driven brand risk without building bespoke infrastructure from scratch.
The Competitive Intelligence Angle: AI as a Brand War Battlefield
Within therapeutic areas where multiple products compete for the same indication, AI-generated comparative information is now a de facto share-of-voice battleground. This isn’t a theoretical future; it’s happening in oncology, immunology, cardiovascular, and the GLP-1 space right now.
Training Data as Competitive Advantage (Accidentally)
AI systems learn from publicly available text. Companies that publish more, publish in more accessible formats, and publish in venues that are heavily indexed generate more training data for AI to draw on. This was not a strategic consideration when those publication decisions were made, but it is becoming one.
A company with a robust real-world evidence publication strategy, active presence in high-traffic medical education websites, and well-cited clinical trial data may find that AI responses about their drug are more accurate and more favorable than responses about a competitor with equivalent or superior clinical data but a less aggressive publication strategy. The clinical quality of the drug is not the only determinant of how AI characterizes it. The depth and accessibility of the published record matters too.
This creates a new, unintended mechanism of competitive disadvantage. If your competitor’s drug has ten times as many published real-world case reports, retrospective analyses, and commentary pieces as yours, AI may generate more detailed, more confident, and more favorable descriptions of their drug even if your randomized trial data is superior. That’s not a data quality issue. It’s a corpus density issue, and it is increasingly a Medical Affairs concern.
Head-to-Head Questions and AI’s Bias Toward Available Data
When a physician asks AI ‘Is drug A or drug B better for [indication]?’ the AI has no access to your internal commercial strategy, your market access data, your differentiation story, or your MSL talking points. It has what’s published. If the published comparative data is equivocal, the AI will say so. If the published data favors your competitor, the AI will say so, regardless of what your brand team says in the field.
In anticoagulation, this played out in the early years of the direct oral anticoagulant class. The published literature on rivaroxaban (Xarelto, J&J/Bayer) and apixaban (Eliquis, Bristol Myers Squibb/Pfizer) generated persistent AI and search-mediated narratives about their comparative bleeding risk profiles that were not fully resolved by later data. The companies’ promotional positions and the AI-generated comparative summaries were often in tension, creating confusion for HCPs trying to make prescribing decisions.
Biosimilar Substitution and the Originator Brand Problem
Biologics facing biosimilar competition have a specific AI vulnerability. As biosimilar availability expands and biosimilar clinical data accumulates, AI training data for those molecules incorporates both originator and biosimilar data. AI responses to questions about adalimumab, for example, increasingly draw on the substantial body of biosimilar clinical data without consistently distinguishing Humira (AbbVie) from the seventeen FDA-approved biosimilars.
For AbbVie, whose brand distinction strategy for Humira in the biosimilar era relied heavily on patient comfort with the established product, AI conflation of originator and biosimilar data is a direct brand problem. A patient who asks an AI whether their Humira prescription could be switched to a biosimilar and why receives a synthesis that may not accurately represent the interchangeability designations of specific products, the state-level substitution laws that govern pharmacy-level switching, or the specific benefit structures that affect net cost.
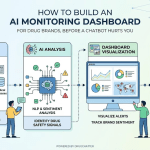
What a Rigorous AI Monitoring Program Looks Like in Practice
For Medical Affairs leaders trying to build a defensible AI monitoring function, the practical requirements are clearer than the vendor landscape might suggest.
Scope: Which Products, Which Platforms, Which Questions
The first decision is scope. Not every drug in a portfolio requires equal AI monitoring intensity. Priority should go to drugs meeting any of these criteria:
- High query volume from HCPs or patients (major indications, primary care-accessible products)
- Complex benefit-risk profiles where AI simplification creates safety risk
- Active competitive market with multiple products in the same indication
- Recent significant label changes (safety updates, new indications, REMS changes)
- Active litigation or post-market safety scrutiny generating heavy media coverage
Platform scope matters too. ChatGPT, Google Gemini, Microsoft Copilot, Meta AI, and Perplexity are the major platforms by user volume and healthcare query share. They have meaningfully different underlying architectures, training data compositions, and update cadences, which means AI responses about your drug can differ substantially across platforms. A monitoring program that only tracks one platform misses significant cross-platform variance.
Query Library Design
The query library, the set of questions you systematically ask AI platforms about your drugs, is the core of the monitoring program. A well-designed query library covers:
- Indication and approved use questions (‘Is [drug] approved for [indication]?’, ‘What is [drug] used for?’)
- Dosing questions, including special populations (renal impairment, pediatrics, elderly)
- Safety and adverse event questions (‘What are the side effects of [drug]?’, ‘Is [drug] safe in pregnancy?’)
- Comparative questions (‘How does [drug] compare to [competitor]?’, ‘Which [drug class] has the best [outcome]?’)
- Off-label use questions specific to known unapproved uses of the drug
- Cost and access questions that may generate payer-relevant misinformation
Queries should be run in both clinical professional framing (‘In a patient with [clinical parameters], what is the recommended dose of [drug]?’) and lay patient framing (‘How much [drug] should I take?’). AI responses can differ meaningfully between these framings, and both matter.
Accuracy Scoring and Labeling Alignment
AI responses need to be scored against a reference standard. The natural reference standard is approved labeling, but in practice, you also need to consider the current version of the label, the jurisdiction (FDA labeling vs. EMA SmPC for European monitoring), and any recent REMS or label updates that may not be reflected in AI training data.
A workable scoring rubric assesses each AI response on four dimensions: accuracy of core clinical claims, completeness of risk information, presence of inappropriate off-label claims, and alignment with current approved labeling language. Responses that score poorly on any dimension trigger a formal gap analysis and content strategy response.
The Feedback Loop: From Monitoring to Action
Monitoring without action is just documentation. The gap analysis from AI monitoring should feed directly into Medical Affairs content strategy. Identified inaccuracies should prompt review of whether labeling language could be clarified. Systematic off-label narrative emergence should trigger MSL field alerts. Competitive disadvantage in AI-generated comparisons should inform the Medical Affairs publication planning cycle.
Companies that close this loop between monitoring and content strategy are beginning to treat AI responses about their products as a managed channel, not a passive outcome. That framing shift, from ‘AI says things about our drug and we can’t control it’ to ‘AI synthesis of publicly available information about our drug is a function of the published record we help create,’ is the practical insight that separates proactive from reactive Medical Affairs teams.
The Patient Safety Dimension No One Is Tracking Systematically
The brand and regulatory risks discussed above are real but manageable through institutional processes. The patient safety dimension is less tractable, because the adverse consequences are distributed and largely invisible to the pharmaceutical industry.
When a patient uses AI to self-triage a medication side effect and receives guidance that delays recognition of a serious adverse event, that outcome rarely traces back to the AI interaction. The patient doesn’t tell their physician ‘ChatGPT told me this was normal.’ The physician doesn’t report an adverse event connected to AI misinformation. The signal never reaches FDA, the company, or anyone with the authority to act on it.
This is a genuine pharmacovigilance gap. The post-marketing surveillance system was built for a world where drug information came from defined, trackable channels. It was not built for a world where drug information comes from a generative AI system that is invisible to the pharmacovigilance infrastructure.
FDA’s 2024-2025 thinking on pharmacovigilance modernization, reflected in the agency’s AI Action Plan released in 2025, acknowledges this gap but does not yet propose a mechanism for closing it. The practical implication for pharmaceutical companies is that they cannot rely on the standard signal detection infrastructure to identify AI-mediated patient safety problems. They have to look for them proactively, which requires the kind of AI monitoring infrastructure described above plus explicit outreach to patient communities where AI misinformation is most likely to propagate.
Rare Disease: The Highest-Risk Intersection
Rare disease patients and caregivers are among the most active users of AI for medical information. The reasons are structural: rare diseases are poorly served by traditional information channels. There are no detail reps for a drug that treats 3,000 patients in the United States. MI call centers may have limited disease-specific expertise. Published information is sparse, technically demanding, and dispersed across specialized journals that patients cannot easily access.
For drugs like nusinersen (Spinraza, Biogen) for spinal muscular atrophy, or migalastat (Galafold, Amicus Therapeutics) for Fabry disease, AI may be the first and most accessible source of information for newly diagnosed families. The accuracy of that information, and its alignment with current dosing, monitoring requirements, and contraindications, has direct clinical consequences for a population with no margin for error.
Monitoring AI outputs for rare disease drugs requires the same framework as for large-market products but with a different calibration of consequences. An AI error in a GLP-1 product description may cause one unnecessary physician visit. An AI error in a rare disease treatment description may contribute to a missed dose escalation or delayed complication recognition in a patient with no alternative therapy.
Where This Goes in the Next Three Years
Predictions in this space are hazardous, but the trajectory of a few dynamics is clear enough to be worth stating.
AI will get better at drug information. The major model developers are actively working on reducing hallucination rates and improving factual grounding. Retrieval-augmented generation (RAG) architectures that ground AI responses in verified, current sources are already being deployed. Google’s integration of health-specific data sources into its AI search products reflects a deliberate investment in medical accuracy. This will not eliminate AI drug information errors, but it will reduce them, particularly for well-documented, high-volume drug queries.
FDA will develop guidance on AI drug information. The agency’s engagement with AI in drug development and promotion has accelerated through 2023 and 2024. The January 2025 AI Action Plan signals that FDA views AI drug information as a regulatory priority. Some form of guidance on company-deployed AI in promotional and MI contexts is likely within the next two years. That guidance will probably draw on the existing OPDP enforcement framework while adding AI-specific requirements around content sourcing, accuracy validation, and post-deployment monitoring.
Pharmaceutical companies that have built AI monitoring infrastructure now will have a structural advantage when FDA guidance formalizes requirements. Companies that wait will be building processes under regulatory deadline pressure. That’s a worse position to be in.
The channel displacement will continue, but not to completion. AI will not replace Medical Information call centers for complex clinical queries requiring nuanced, evidence-based responses. It will not replace face-to-face MSL interactions for scientific exchange. What it will do, and is already doing, is absorb the high-volume, lower-complexity queries that previously went to the MI call center or to the package insert. That volume shift has downstream consequences for how companies staff and prioritize their medical information functions.
Key Takeaways
- AI chatbots are already displacing traditional drug information channels at scale, with measurable effects on how physicians, patients, and payers form drug knowledge before engaging any official channel.
- The error rate in AI drug responses is clinically significant. A 26% inaccuracy rate in peer-reviewed analysis of LLM medication responses is not an acceptable quality standard for information reaching clinical decision-makers.
- FDA’s regulatory framework has a gap. The agency regulates what companies say about their drugs, not what AI systems say. The gap between those two scopes is where most current AI drug information risk lives.
- Brand risk and regulatory risk are distinct problems requiring different responses. Brand risk is managed through content strategy. Regulatory risk is managed through governance of company-deployed AI tools and compliance infrastructure.
- Rare disease patients are most exposed to AI drug information errors because traditional channels serve them poorly and AI use is disproportionately high in this population.
- The companies building AI monitoring infrastructure now are not just managing current risk — they are positioning themselves to comply with FDA guidance before it is issued as a deadline, rather than after.
- AI synthesis of drug information is a function of the published record. Medical Affairs teams that understand this can treat publication strategy as an active lever for shaping AI outputs, not just scientific communication.
Frequently Asked Questions
If a company doesn’t deploy AI tools itself, does it still have regulatory exposure from AI-generated drug information?
Largely no, for now. FDA’s promotional regulations apply to manufacturers and their agents. An AI platform generating inaccurate drug information without any relationship to the manufacturer is outside OPDP’s current enforcement jurisdiction. The exposure changes if the company has done anything to actively feed content into AI training pipelines, endorses AI-generated content, or uses AI-generated outputs in its own promotional activities. For most companies, the primary current exposure is internal: AI tools deployed by the company itself, particularly in patient-facing or HCP-facing customer engagement, are subject to standard promotional requirements regardless of whether a human or an algorithm generated the specific output.
How often do major AI platforms update their training data for drug information?
This varies by platform and is not consistently disclosed. GPT-4-based systems operate on training data with cutoffs that have ranged from early 2023 to late 2024 depending on the model version, and retrieval-augmented features that pull from current web sources are inconsistently applied in clinical queries. Google’s Gemini products have more aggressive real-time data integration through their search stack, which can mean more current label information but also more exposure to recent adverse event coverage. Perplexity’s architecture emphasizes current web retrieval over static training data. The practical implication is that training data cutoffs are not a reliable protection against AI drug information errors, but they are a consistent source of errors around recent label changes, new approvals, and evolving safety data.
Are there documented cases where FDA has taken action specifically related to AI-generated drug promotion?
As of early 2025, there are no public Warning Letters or Untitled Letters from OPDP specifically citing AI-generated content as the primary violation. There are enforcement actions against digital promotional content that could have been AI-assisted, but OPDP letters describe the content violation, not the production mechanism. The first AI-specific enforcement action will likely come from a company-deployed chatbot or AI representative tool that makes an efficacy claim unsupported by labeling, or omits required risk information. Given that several large pharmaceutical companies have deployed or are piloting AI-driven customer engagement tools, that first action is probably a matter of timing rather than probability.
Can pharmaceutical companies influence what AI says about their drugs without violating promotional regulations?
Yes, through several mechanisms that are clearly outside promotional regulations. Publishing peer-reviewed clinical data in accessible, well-indexed journals improves AI training data quality without any promotional intent. Maintaining accurate, current, and clearly written public-facing content on company and drug websites helps AI retrieve-and-summarize pipelines access correct information. Working with recognized medical education organizations to produce accurate, label-aligned content adds to the legitimate medical literature AI draws from. What companies cannot do is try to game AI systems through undisclosed content seeding, astroturfing tactics, or paying third parties to produce content favorable to their products, all of which carry existing legal and regulatory risk independent of AI context.
What is the most common category of AI drug information error that Medical Affairs teams are finding when they audit AI outputs?
The most common category, based on published evaluations and reports from Medical Affairs professionals at industry conferences, is temporal accuracy: AI providing dosing, contraindication, or indication information that was correct at some point but reflects an older version of the label rather than the current approved prescribing information. This is distinct from hallucination, which involves fabricated information, and from synthesis errors, which involve mixing information from different drugs or different formulations. Temporal accuracy errors are particularly pernicious because the information was once true, which means it exists in the training corpus with full credibility and nothing in the AI’s response signals that it might be outdated. These errors cluster around drugs with recent label updates, reformulations, or newly identified safety signals where a significant body of pre-update content exists in AI training data.
Sources and references: Veeva Pulse Field Trends Report 2024. Khullar D, et al., JAMA Network Open 2024 on AI medication query accuracy. FDA AI Action Plan, January 2025. Medical Affairs Professional Society (MAPS) AI Survey 2024. FDA Draft Guidance on Electronic Systems for Adverse Event Reporting, 2023. JAMA Internal Medicine 2023, ChatGPT-3.5 accuracy evaluation on medication queries. FDA 21 CFR Parts 201, 202; FD&C Act Section 502. OPDP Warning Letters, 2022-2023 (Genentech, Sanofi, AstraZeneca). FDA Discussion Paper on AI/ML in Drug Development, January 2024.
This article does not constitute legal or regulatory advice. Pharmaceutical companies should consult qualified regulatory counsel regarding AI deployment in promotional and Medical Information contexts.