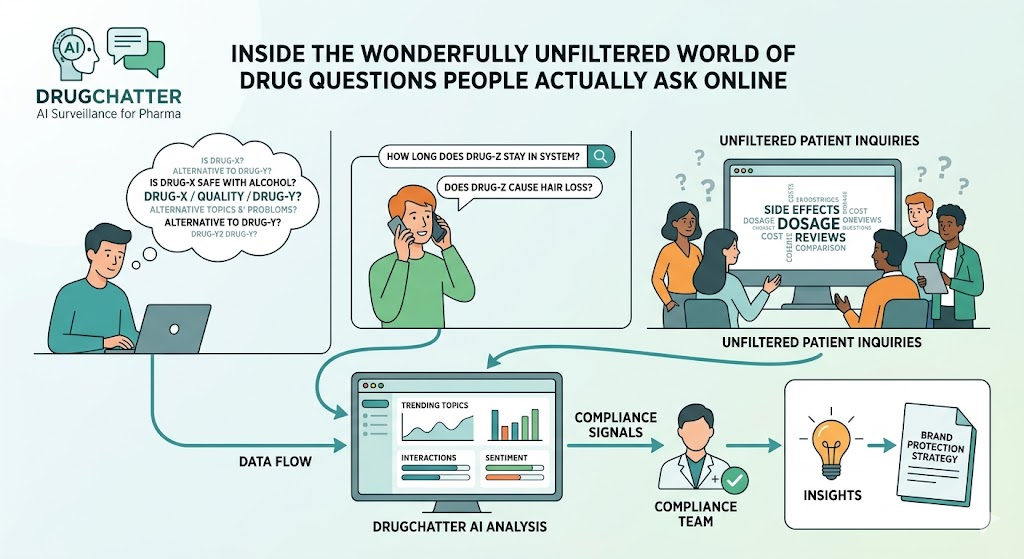
Inside the wonderfully unfiltered world of drug questions people actually ask online
Spend enough time around pharmaceutical R&D and you start to believe medicine is a neat, orderly system: receptors, pathways, endpoints, hazard ratios. Then you spend five minutes reading public drug forums and remember what healthcare actually looks like in the wild.
People are not asking abstract pharmacology questions. They’re trying to figure out whether grapefruit oil will sabotage their statin. Whether Ozempic changes how apples taste. Whether mushroom supplements, onion supplements, yoga supplements, aspirin, fish oil, or melatonin are about to collide with their prescriptions in some unholy CYP450 pileup.
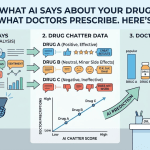
That’s what makes the questions on DrugChatter so revealing. They expose the real interface between modern medicine and everyday life.
And some patterns emerge very quickly.
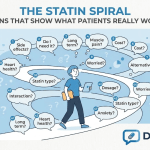
1. Lipitor has become the internet’s most interrogated molecule
No drug in this batch attracted more “can I combine this with that?” anxiety than atorvastatin.
Patients wanted to know:
- Can avocado Lipitor interaction cause harm?
- Does grapefruit enhance Lipitor’s effectiveness?
- Can grapefruit oil reduce Lipitor’s cholesterol benefits?
- Can lavender oil affect Lipitor’s cholesterol-lowering ability?
- Can high chlorine levels in pools reduce Lipitor’s benefits?
- How do iron-rich foods impact Lipitor’s effectiveness?
- Can I consume almond milk while on Lipitor?
This is the post-statins era in miniature. Lipitor is no longer viewed as “a pill.” It’s viewed as a participant in a sprawling biochemical ecosystem involving smoothies, supplements, gym routines, antihistamines, and apparently swimming pools.
Some of these concerns are pharmacologically plausible. Grapefruit interactions with statins are well established. Others are more speculative. But that’s almost beside the point.
Patients increasingly assume everything interacts with everything else. And honestly, after years of hearing drug disclaimers delivered at auctioneer speed in TV commercials, you can see how we got here.
2. Ozempic has escaped endocrinology and entered culture
The GLP-1 class now occupies the same strange territory once held by Prozac or Viagra: part medicine, part cultural phenomenon.
The questions reflect that shift immediately:
- Can Ozempic enhance workout results for weight loss?
- Does Ozempic interact with certain foods?
- Is fruit consumption including apples affected by Ozempic?
- Can Mounjaro cause sulfur burps worse than Ozempic?
- What should I do if I miss my semaglutide injection?
- What’s the difference between Wegovy and Ozempic for weight loss?
The sulfur-burps question deserves special recognition because it captures the modern pharmaceutical internet perfectly: highly specific, slightly alarming, and impossible to imagine appearing in a medical textbook twenty years ago.
These drugs are no longer confined to diabetes clinics. They’ve become lifestyle infrastructure. People now evaluate them the way consumers evaluate operating systems.
3. The supplement economy has created pharmacological chaos
If there’s a dominant theme running through these questions, it’s this:
People desperately want natural products to coexist peacefully with prescription medicine.
Sometimes that means plausible combinations:
- Is it safe to take a cinnamon supplement for my blood sugar?
- Can you take magnesium with levothyroxine?
- Can I take magnesium with gabapentin?
- Can gut bacteria impact Vascepa’s therapeutic response when combined with probiotics?
And sometimes the internet wanders into surrealist territory:
- Can I take an onion colorful supplement for my nutrition?
- Can I take an onion periodic supplement for my health?
- How long does it take for an onion monochrome supplement to work?
I have many questions about the onion supplement universe, and none of them have answers.
But there’s a serious point underneath the weirdness: supplements increasingly occupy the same psychological category as medicine. Consumers expect them to produce measurable physiological effects. Which means they also worry — reasonably — about interactions.
4. “Natural” does not mean “safe,” and users know it
One of the more encouraging patterns here is how often users are actively skeptical about supplements and wellness products.
Examples:
- Can green tea extract cause liver damage?
- Is it safe to take a turkey tail mushroom supplement for my immune system?
- Is it safe to take a Ginkgo Biloba supplement for my memory?
- Can aloe vera juice help with acid reflux?
- Does boron affect testosterone levels?
This is the collision between the wellness industry and evidence-based medicine. Consumers are simultaneously intrigued by alternative therapies and suspicious of them. Which is probably healthier than blind optimism.
5. The real obsession isn’t efficacy. It’s interaction risk.
Read enough of these questions and something becomes obvious: patients are often less worried about whether a drug works than whether it quietly collides with the rest of their lives.
That’s why interaction questions dominate:
- Is it safe to take Xanax and clonidine?
- Can I take Tylenol with hydrochlorothiazide?
- Does oxycodone interact with benzodiazepines?
- Can methotrexate cause adverse effects with NSAIDs?
- Can I drink grapefruit juice while taking verapamil?
- Can combining Tylenol, Advil, and Lipitor lead to increased liver risks?
This is modern polypharmacy anxiety. People aren’t taking one drug anymore. They’re taking six prescriptions, three supplements, caffeine, protein powder, melatonin gummies, and occasionally “immune support” capsules purchased from a podcast ad.
No physician visit has enough time to fully model that reality.
6. DrugChatter reveals something pharma companies rarely see
The industry spends billions studying clinical endpoints. But these questions reveal the endpoint patients actually care about:
“Can I still live normally while taking this?”
Can I eat grapefruit?
Can I drink occasionally?
Can I work out?
Can I take vitamins?
Can I combine this with allergy medicine?
Can I survive Thanksgiving dinner without triggering a metabolic catastrophe?
That’s the real-world layer sitting underneath every prescribing decision.
And in a strange way, the most revealing questions are the oddest ones.
Because nobody asks whether chlorine pools interfere with Lipitor unless medicine has become deeply embedded in daily identity. The drug is no longer a temporary intervention. It’s part of the operating system of life.
Which means patients start interrogating every input. Every food. Every supplement. Every routine.
The internet may not always produce clean pharmacology.
But it produces honest questions.